Can Dentures Be Fitted to Receding Gums? A Complete Guide
Yes, dentures can be fitted to receding gums. The harder truth is that receding gums change the shape of the gum line, reduce tissue support, and often come with bone loss, so the fit usually needs more planning and more follow-up than a routine case. Traditional dentures can still work for many patients, but some people do better with soft liners, frequent adjustments, or implant-supported dentures when gum recession affects stability too much.
The right answer depends on three things: how much gum recession you have, whether gum disease is still active, and how much jawbone support is left. That is why two patients with the same question can get very different treatment plans. One patient may do well with custom dentures. Another patient may need gum disease treatment, a gum graft, bone grafting, or dental implants before long-term tooth replacement becomes stable.
Table of Contents
Understanding Gum Recession
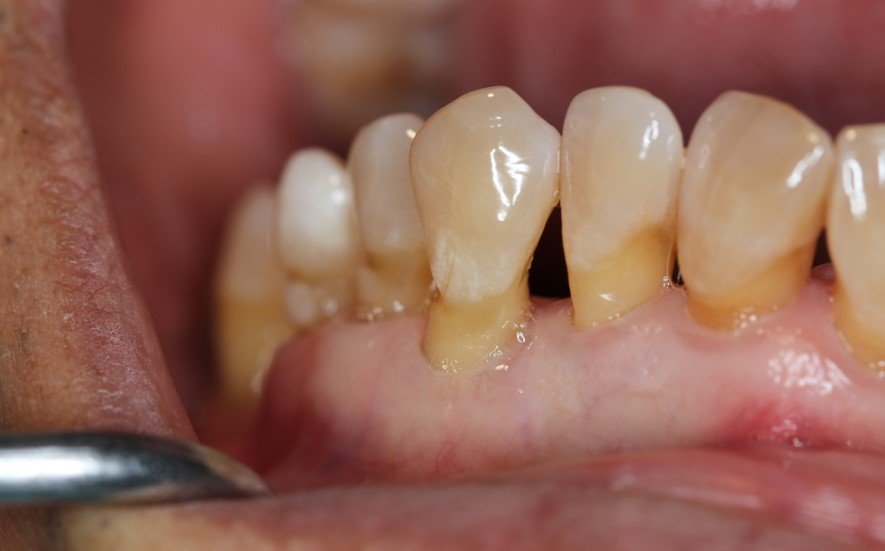
Gum recession, also called gingival recession, happens when gum tissue pulls away from the teeth and exposes the tooth root. Gum recession often starts with plaque, bacteria, and gum disease, but it can also be linked to aggressive brushing, tobacco use, tooth position, or thin tissue. Once recession starts, the roots become more sensitive, the gum line becomes uneven, and the supporting bone can shrink too.
That matters for dentures because dentures sit on oral tissue, and full dentures rely on the gums and underlying bone for support. If the tissue is uneven or the jawbone has shrunk, denture plates have less stable contact with the mouth. That is where fitting challenges start. Patients often describe loose dentures, rubbing, poor suction, or pressure on sensitive spots.
Can Dentures Be Fitted to Receding Gums?

Yes, dentures can be fitted to receding gums, and dentists do it all the time. But dentures can absolutely be fitted to receding gums only when the provider plans around the recession instead of pretending the gum contours are normal. Traditional dentures depend on fit, suction, and sometimes adhesive. Receding gums dentures cases work best when the dentures are made around the current shape of the gums and then checked again as the mouth changes.
This is why custom-fitted dentures matter. Dentures are custom-made from impressions of your gums, and in harder cases the dentist may use multiple impressions, a digital scanner, or 3D imaging when implant-supported options are on the table. That gives the dental team a clearer view of unique gum contours, irregular gum surfaces, and bone structure before they lock in the treatment plan.
The Reality of Long-Term Success
The long-term issue is not whether a denture can be fitted once. The real issue is whether the mouth stays stable enough for that fit to last. Gum recession affects denture fitting over time because active gum disease, alveolar bone loss, and normal age-related shrinkage can keep changing the shape of the gums and jawbone. When that happens, even a good denture can become loose later.
That is why long-term success depends on stopping the cause of the recession, not just replacing teeth. If gum disease is still active, dentures may keep losing stability. ADA guidance states that a denture that fits poorly may need to be relined or replaced, and ill-fitting dentures can cause mouth sores and, with prolonged use, bone loss.
Dentures For Receding Gums
Dentures for receding gums can still restore appearance, chewing, and speech. They can replace missing teeth, support facial shape, and give a patient a removable tooth replacement option without surgery. In the UK or elsewhere, the basic principle stays the same: dentures fit over the gums to replace missing teeth, but the fit needs monitoring as the mouth changes.
Advantages
The first advantage is access. Traditional dentures are usually less invasive and less expensive than dental implants. The second advantage is flexibility. Dentists can adjust, reline, rebase, or remake dentures as the gum line changes. The third advantage is that modern denture materials and soft-liner dentures can improve comfort on sensitive tissue and irregular gum surfaces.
For some patients, dentures are the only realistic short-term answer after extractions. Immediate denture placement can replace teeth on the same day they are removed, which helps protect appearance during healing. That can matter a lot for confidence, speech, and day-to-day function.
Disadvantages
The biggest disadvantage is stability. Receded gums and bone loss reduce the foundation that traditional dentures need. NHS guidance says dentures may become loose as the gums and jawbone shrink or change shape, and that can affect eating and speaking.
The second problem is irritation. Ill-fitting dentures can rub the tissue, create sore areas, and push patients to use more adhesive instead of fixing the fit. Adhesive can help some people, but it is not a repair. If the denture is loose, the answer is adjustment, relining, rebasing, or replacement, not endless adhesive.
Addressing Challenges with Denture Fitting
Fitting challenges receded gums cases usually come down to support, comfort, and maintenance. The dentist has to work around uneven tissue, reduced suction, and pressure points on sensitive areas. That often means more than one adjustment after the first fit. New dentures often create sore spots at first, and Leeds Teaching Hospitals advises follow-up adjustments to correct uncomfortable areas.
The first fix is not always a new denture. A dentist may reshape pressure areas, add a soft lining, or reline the base so the denture matches the current gum contours better. Over time, dentures can also be rebased or remade if the base or teeth are too worn. That is the practical answer to questions like can dentures be refitted, can dentures be tightened up, or can dentures be fixed to fit better. Yes, often they can, but only after a proper examination.
The second fix is disease control. If gum recession comes from gum disease, the infection has to be treated. NIDCR explains that periodontitis destroys the bones, gums, and tissue that support teeth. A periodontist may recommend scaling and root planing, surgery, extractions, gum grafts, or bone grafting depending on the damage.
Advanced Options: When Traditional Dentures Aren’t Enough
Some mouths are too unstable for traditional dentures to work well for long. That does not mean you are out of options. It means the foundation needs to change. This is where an Implant Specialist, prosthodontist, periodontist, or oral surgeon may shift the conversation from suction-based dentures to implant-supported options or grafting procedures.
Implant-Supported Dentures: The Game-Changer
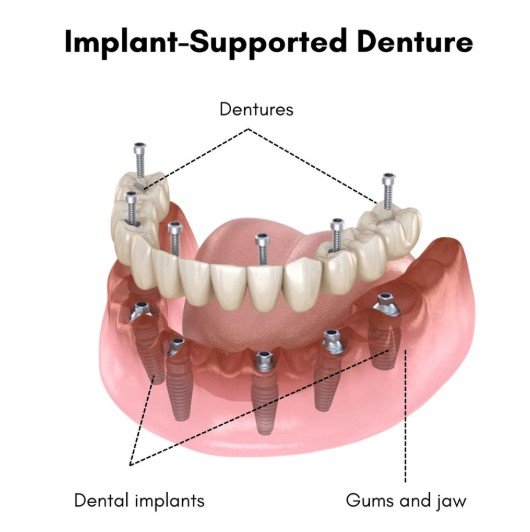
Implant-supported dentures attach to titanium implants in the jawbone instead of resting only on the gums. Cleveland Clinic states that implant-supported dentures offer more stability than traditional dentures and improve chewing, eating, and speaking. They can be removable or fixed, and fixed versions often feel far more secure.
This matters even more when gum recession is severe. Implants act like a new tooth root inside the bone, so the denture no longer depends only on weak suction over compromised tissue. Implant-supported dentures can reduce slipping, and Cleveland Clinic notes they help prevent bone loss in the jaw. All-on-4 treatment is one version of this approach, where an entire arch is supported by four implants.
Not every patient qualifies right away. You need enough bone for implant placement, and some cases need bone grafting first. Still, when traditional dentures are unstable, this is often the strongest long-term option. Mayo Clinic notes that dental implant surgery can be helpful when dentures fit poorly or when there are not enough natural teeth roots to support a denture plan.
Bone Grafting: Rebuilding Your Foundation
Bone Grafting rebuilds lost support with bone material in areas where the jawbone has thinned. A periodontist may place a dental bone graft when periodontal infection has eroded the bone that supports the teeth, and Cleveland Clinic notes that bone grafts can add volume and density for later implant-supported dentures.
Bone grafting does not make every patient an implant candidate overnight. Healing takes time, and the plan depends on scan results, the shape of the bone structure, and overall health. But if alveolar bone loss is the main reason dentures keep failing, rebuilding the foundation can change the whole result.
Gum Grafts
Gum grafts treat the soft-tissue side of recession. Cleveland Clinic describes gum graft surgery as a procedure that covers exposed tooth roots and adds volume to the gum line. A periodontist places tissue in the receded area to improve coverage and comfort.
A gum graft is not a replacement for a denture and not a substitute for bone. But it can help when the gum line is thin, sore, or uneven and the tissue needs rebuilding before or during broader treatment. In some patients, gum grafts improve comfort around remaining teeth. In other patients, extractions and full tooth replacement make more sense. The decision is case by case.
What to Expect During Your Denture Fitting Process

The denture fitting process is not one quick visit. It is a staged process that starts with diagnosis and ends with adjustments. The more recession and bone loss you have, the more planning usually goes into it.
Initial Consultation and Assessment
The first visit usually includes a full oral exam, a review of your teeth, gums, tissue, and bite, and impressions of your mouth. Cleveland Clinic notes that dentures are made from impressions of the gums and any remaining teeth, and NHS guidance says dentures are custom-made from mouldings of the gums. If implants are being considered, the dentist may add x-rays or 3D scans to assess the jawbone.
Treatment Planning
Treatment planning turns the exam into a real plan. That plan may include gum disease treatment, Extractions, Immediate denture placement, Implant placement, or a referral to an Implant Specialist or periodontist. Mayo Clinic’s dental specialties page shows why this can involve more than one type of dentist: periodontics handles bone and gum disease and regenerates soft tissue, while prosthodontics restores missing teeth with removable dentures or dental implants.
The Fitting Process
The fitting process for custom dentures often includes an initial impression, a more detailed second impression, a bite record, a try-in stage, and then the final fit. Leeds Teaching Hospitals describes these stages for complete dentures, and follow-up reviews are used to adjust sore spots and refine the fit. With receding gums, those review visits matter more, not less.
Addressing Common Concerns About Dentures and Gum Recession
Most patients do not ask technical questions first. They ask practical ones. That makes sense.
“Will my dentures fall out?”
They should not fall out when they are properly fitted, but traditional dentures can loosen as gums and the jawbone change shape. NHS guidance says exactly that. Implant-supported dentures are the most secure option because they attach to implants instead of depending only on suction over the gums.
“Will it hurt with my sensitive, receded gums?”
Some soreness is common at the start. Leeds Teaching Hospitals says sore spots in the mouth are common after fitting, and the dentist adjusts the pressure areas at follow-up. Receded gums can be more sensitive, so soft-liner dentures or extra adjustment visits may help. Persistent pain is not normal. Persistent pain usually means the fit needs correction.
“Can I eat normally?”
You may need dietary adjustments at first. Leeds guidance for immediate dentures suggests starting with softer foods early on. Traditional dentures often take time to master, especially with lower dentures. Implant-supported dentures usually give stronger chewing stability and fewer food restrictions.
Making the Right Choice for Your Situation
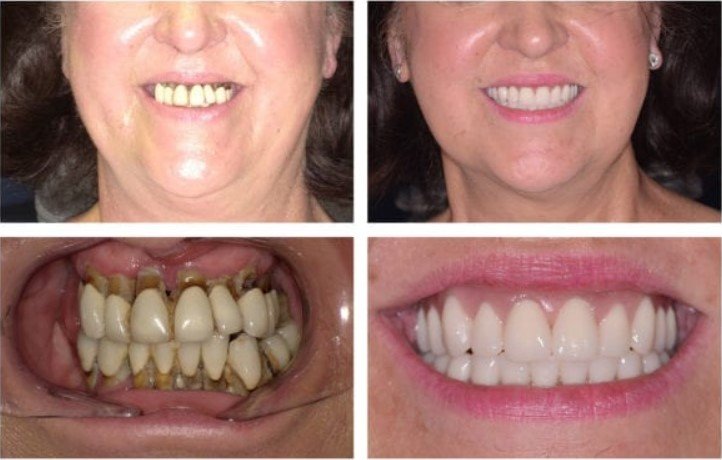
The right choice depends on what you want and what your mouth can support. If recession is stable, the tissue is reasonably healthy, and the jawbone still gives support, traditional dentures may be enough. If the recession is advanced, the bone is weak, or you are tired of loose dentures, implant-supported dentures may be the better long-term answer.
This is where patients get misled. “Can gums recede too much for dentures?” is the wrong question. The better question is whether traditional dentures are still the best option for that level of gum recession and bone loss. Sometimes the answer is yes. Sometimes the honest answer is no, and the better plan is grafting or implants.
Your Next Steps
Book a full denture and gum assessment with a dentist who deals with complex denture fitting, gum recession, or implant-supported options. Ask what is causing the recession, whether gum disease treatment is needed first, how much bone is left, and whether your current dentures are candidates for adjustment, relining, or replacement.
Do not try to reshape, reline, or repair dentures at home. Poor self-adjustment can make the pressure worse and speed up tissue and bone problems. Keep regular reviews even after the dentures feel fine, since ADA and NHS guidance both stress that denture fit changes over time.
Conclusion
Yes, dentures can be fitted to receding gums, and dentures can absolutely work in many cases. But gum recession affects denture fit, comfort, and long-term stability, so the approach has to match the condition of the gum line, tissue, and jawbone. Custom-fitted dentures, soft-liner dentures, relines, and periodic adjustments can solve a lot. They do not solve everything.
When traditional dentures are not stable enough, fitting dentures advanced options such as implant-supported dentures, Bone Grafting, or gum grafts may give a better foundation. That is the real answer to receding gums dentures problems: not false hope, not blanket rejection, just the right treatment for the mouth in front of the dentist.