Dental Bone Loss Treatment: Best Options to Save Your Smile
Dental bone loss can sound alarming, but it is treatable in many cases. The key is finding the cause early and choosing the right treatment before the damage becomes more severe. In simple terms, dental bone loss happens when the jawbone that supports your teeth starts to shrink or break down. This most often happens because of advanced gum disease, missing teeth, infection, trauma, or long-term pressure changes in the mouth. Untreated periodontitis can damage the soft tissue and the bone supporting teeth, which may eventually lead to loose teeth or tooth loss.
For readers searching for practical answers, the good news is this: there is no single “one-size-fits-all” dental bone loss treatment. Dentists and specialists choose treatment based on how much bone has been lost, what caused it, whether infection is still active, and whether the goal is to save natural teeth, prepare for implants, or rebuild the jaw for function and appearance. In this article, we’ll guide you through everything you need to know about dental bone loss treatment, from early detection to recovery and prevention.
Table of Contents
What Is Dental Bone Loss?
Dental bone loss refers to the loss of the alveolar bone, the part of the jawbone that surrounds and supports your teeth. Healthy bone stays active when teeth and gums are healthy and when chewing forces stimulate the jaw. But when gum disease destroys supporting tissues, or when a tooth is lost and not replaced, the bone can begin to resorb over time. Periodontitis is a serious gum infection that can destroy the bone supporting teeth, while untreated tooth decay or infection can also spread damage into the surrounding bone.
Many people do not notice bone loss right away because it often progresses slowly. You may first notice gum recession, loose teeth, changes in your bite, or difficulty chewing. In some cases, the bone loss is first seen on dental X-rays during a routine exam.
Main Causes of Jaw Bone Loss Around Teeth
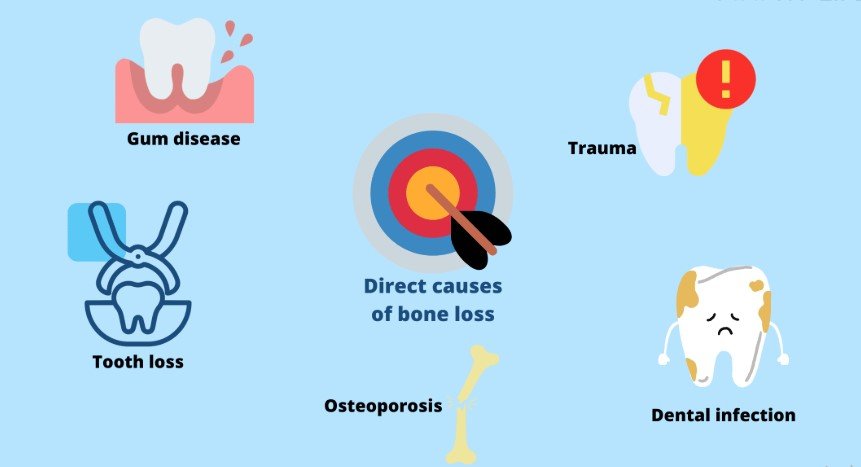
Understanding the cause is the first step in choosing the best dental bone loss treatment.
Periodontal disease
This is the most common cause. Gum disease starts as gingivitis, which causes red, swollen, or bleeding gums. Gingivitis itself does not cause bone loss, but if left untreated it can progress to periodontitis, which can destroy the bone and connective tissues that hold teeth in place.
Missing teeth
When a tooth is removed or lost and not replaced, that area of the jaw no longer gets normal chewing stimulation. Over time, the body may begin to resorb the bone there. This is one reason bone grafting is often recommended before implant placement.
Dental infections and abscesses
Untreated cavities, root infections, or abscesses can spread beyond the tooth and damage nearby bone.
Trauma or injury
An accident, facial injury, or bite trauma can damage the bone around teeth and affect long-term stability.
Denture pressure and bite changes
Poorly fitting dentures and abnormal bite forces can contribute to changes in the underlying bone over time.
Signs You May Need Dental Bone Loss Treatment
Because bone loss often advances quietly, watch for these warning signs:
- Bleeding, swollen, or tender gums
- Gum recession or “longer-looking” teeth
- Persistent bad breath
- Loose teeth
- Pain while chewing
- Changes in how teeth fit together
- A sunken appearance in areas where teeth are missing
These signs can point to gum disease or another issue affecting the supporting bone, and they warrant a dental exam. NIDCR notes that gum disease can spread to the bones surrounding the gums, causing pain with chewing and loose teeth in severe cases.
How Dentists Diagnose Bone Loss
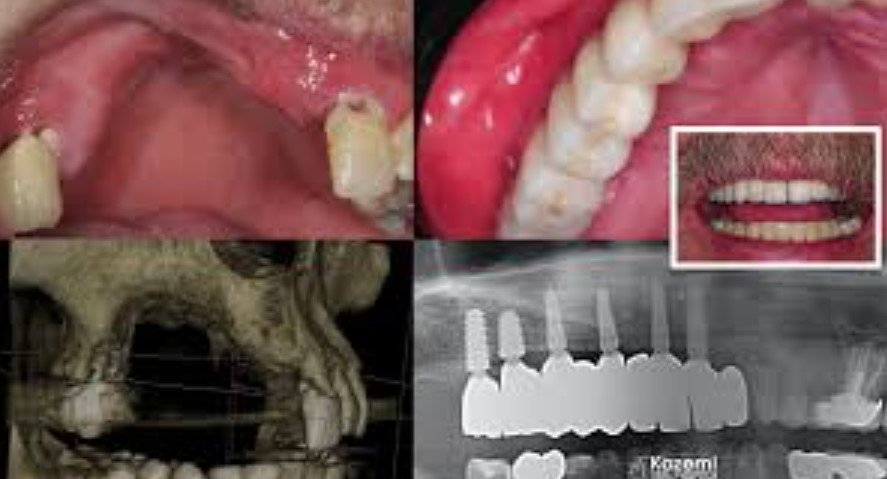
Diagnosis usually includes a gum exam, probing around the teeth, and dental X-rays. Dentists measure periodontal pockets and check whether supporting structures have already been damaged. NIDCR notes that severe periodontitis is assessed using measures such as clinical attachment loss and periodontal probing depth.
In more complex cases, a periodontist or oral and maxillofacial surgeon may order 3D imaging to evaluate the amount and shape of remaining bone before recommending surgery, grafting, or implants.
The Best Dental Bone Loss Treatment Options
Treatment depends on whether the goal is to stop ongoing destruction, rebuild lost bone, or both.
1) Deep Cleaning for Early to Moderate Disease
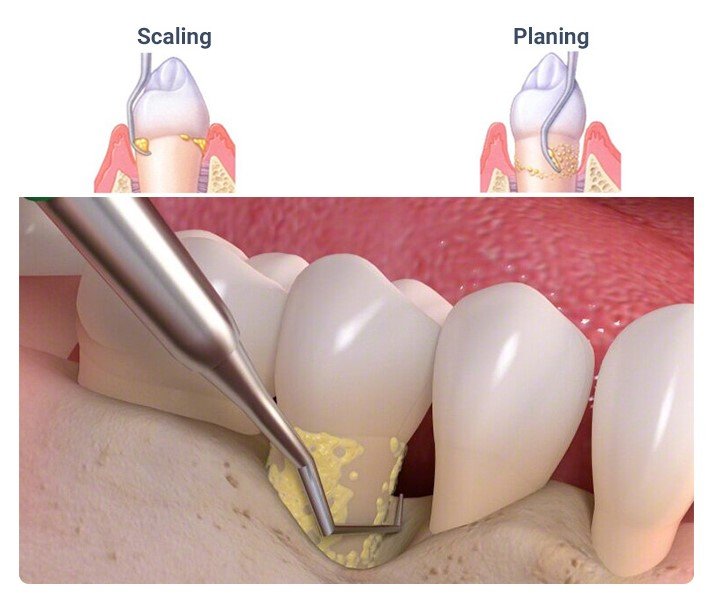
If bone loss is related to gum disease and caught early enough, scaling and root planing, often called deep cleaning, may be the first step. This treatment removes plaque and tartar below the gumline so the gums can heal and inflammation can decrease. It does not regrow large amounts of lost bone by itself, but it can help stop the disease process and preserve remaining bone. Mayo Clinic lists scaling and root planing among core treatments for periodontitis.
This option works best when bone loss is mild to moderate and infection has not become too advanced.
2) Antibacterial and Supportive Therapy
Some patients also need antimicrobial rinses, localized antibiotics, or other supportive care to control infection and reduce pocket depth. These treatments are often paired with professional cleanings and improved home care, not used as standalone fixes.
3) Periodontal Surgery
When deep pockets remain after non-surgical treatment, periodontal surgery may be needed. Flap surgery, also called pocket reduction surgery, allows the specialist to lift the gums, remove deeper tartar deposits, and smooth damaged areas more effectively. Mayo Clinic notes that underlying bone may be reshaped during surgery when periodontitis has caused bone loss.
This treatment aims to reduce bacterial buildup, improve cleanability, and slow or stop further destruction.
4) Bone Grafting to Rebuild Lost Jawbone
Bone grafting is one of the most important treatments for moderate to severe dental bone loss. A dental bone graft replaces missing or lost bone in the jaw and is commonly used when bone loss affects oral health or when more bone is needed before implant placement. Cleveland Clinic explains that initial healing may take about a week, while full graft maturation can take much longer.
Bone graft material may come from your own body, a donor source, or a synthetic material. In broader bone grafting, Cleveland Clinic identifies autograft, allograft, and synthetic grafts as common approaches.
Bone grafting may be recommended for:
- Bone loss from periodontitis
- Areas where a tooth was extracted
- Preparing the jaw for implants
- Ridge preservation or ridge augmentation
- Rebuilding areas beneath the sinus in the upper jaw
5) Ridge Preservation After Extraction
If a tooth must be removed, your dentist may recommend placing graft material immediately into the socket. This is called ridge preservation. The goal is to reduce post-extraction bone shrinkage and make future tooth replacement easier.
6) Sinus Lift for Upper Back Teeth
When the upper jaw does not have enough bone height for implants, a sinus lift may be performed to create space for additional grafting material. This is often needed in the back upper jaw where natural bone can be limited.
7) Dental Implants After Bone Regeneration
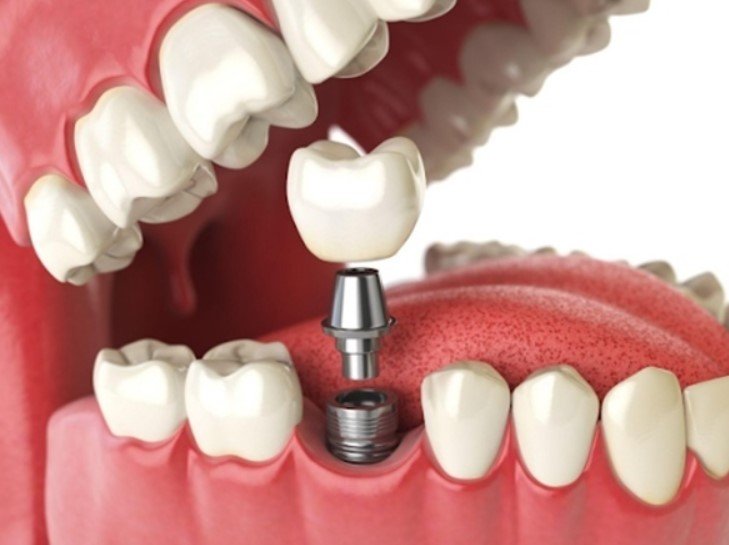
If bone loss happened because a tooth was missing, a dental implant may be the long-term replacement after the site is rebuilt. Cleveland Clinic notes that when there is not enough bone for immediate implant placement, bone grafting may be needed first and healing may take months before the implant is placed.
Implants can help restore chewing function and may help maintain bone by restoring stimulation to the jaw.
Can Lost Dental Bone Grow Back Naturally?
This is a common question, and the honest answer is: significant dental bone loss usually does not fully grow back on its own. Early disease can sometimes stabilize with treatment, and some regenerative procedures can encourage new bone formation in specific cases, but established bone loss usually needs professional treatment. That is why early diagnosis matters so much.
Which Specialist Treats Dental Bone Loss?
You may start with a general dentist, but many patients are referred to:
- A periodontist for gum disease and supporting bone issues
- An oral and maxillofacial surgeon for grafting, extractions, advanced reconstruction, or implant surgery
AAOMS notes that oral and maxillofacial surgeons are experienced in bone grafting and implant-related surgery.
Recovery and Healing Timeline
Healing depends on the treatment. Deep cleaning recovery is usually short, while surgical treatment and bone grafting take longer. Cleveland Clinic states that initial healing after a dental bone graft may take about a week, but complete healing can take much longer, sometimes many months depending on the case. Implant treatment may also involve staged healing before the final restoration is placed.
Your dentist may recommend a soft diet, excellent oral hygiene, follow-up visits, and avoiding smoking during healing.
How to Prevent Future Bone Loss
Prevention is often simpler than reconstruction. Good brushing and flossing habits help prevent plaque buildup that can trigger gum disease. NIDCR states that gum disease is typically caused by plaque buildup and poor brushing and flossing habits. Mayo Clinic and NIDCR also note that smoking is a major risk factor, and overall health conditions such as diabetes can worsen oral problems.
The best prevention steps include:
- Regular dental cleanings and exams
- Treating gingivitis early
- Replacing missing teeth when appropriate
- Avoiding tobacco
- Managing diabetes and other health conditions
- Wearing appliances or dentures that fit properly
Also Read: Nature’s Smile Gum Balm Reviews: Can This Natural Formula Really Help Your Gums?
When to See a Dentist Right Away
Do not wait if you have loose teeth, pus around the gums, facial swelling, pain while chewing, or a sudden change in your bite. These can point to active infection or advanced periodontal damage that needs prompt treatment.
Trusted Resources
- NIDCR (National Institute of Dental and Craniofacial Research) for gum disease basics and research-backed oral health information.
- Mayo Clinic for symptoms, causes, and treatment overviews of periodontitis.
- Cleveland Clinic for patient-friendly guides on dental bone grafts and implants.
- AAOMS for information related to oral and maxillofacial surgery, grafting, and implants.
Final Thoughts
The right dental bone loss treatment can stop disease, protect remaining teeth, and in many cases rebuild support for a healthier smile. Mild cases may improve with deep cleaning and periodontal care, while more advanced cases may need surgery, bone grafting, or implants. The earlier you act, the more treatment options you usually have. If you suspect gum disease or jawbone loss, booking a dental evaluation early can make all the difference.