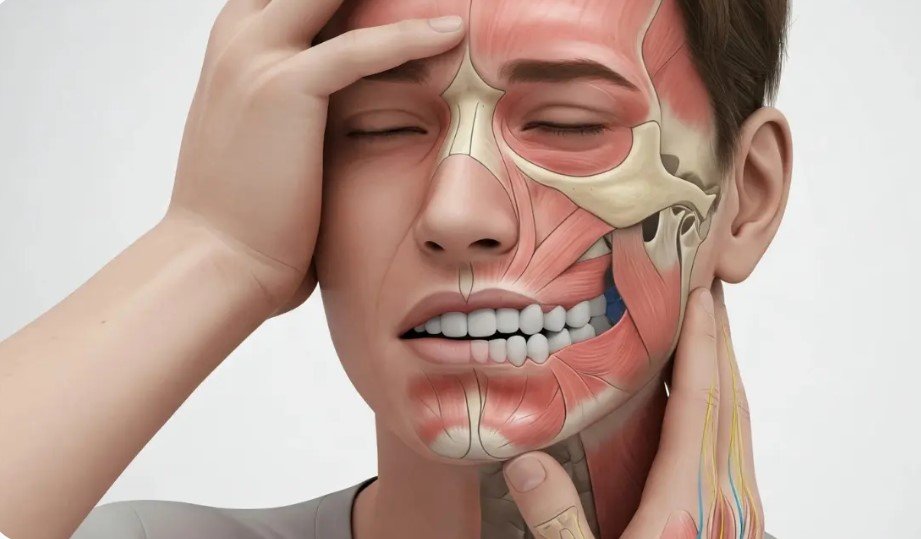
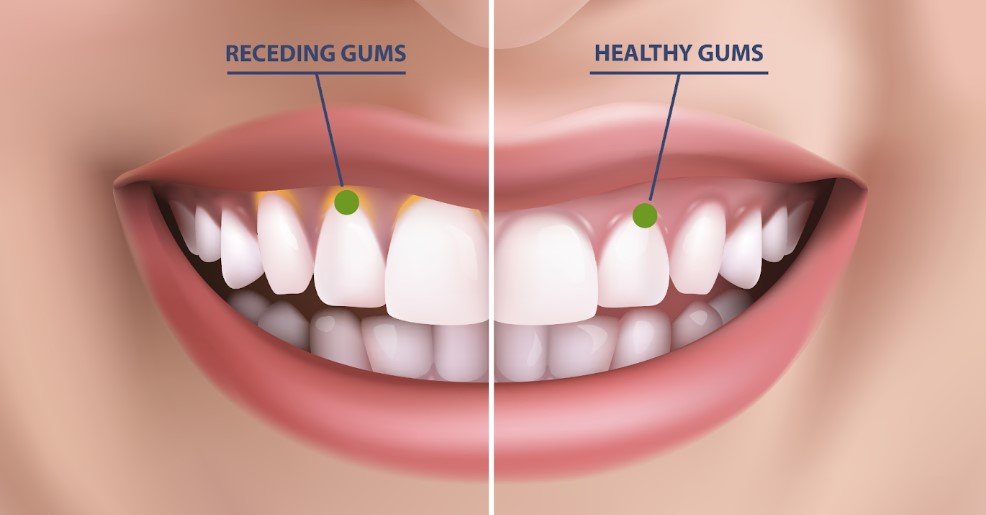
Gum Disease Headache: Can Unhealthy Gums Trigger Head Pain?
If you have sore gums and a nagging headache at the same time, it is natural to wonder whether the two are connected. The short answer is that gum disease is not usually listed as a classic “headache disorder,” but gum inflammation, infection, painful chewing, jaw discomfort, and dental abscesses can contribute to pain that feels like it spreads into the head, face, or jaw area. Gum disease commonly causes red, swollen, tender, or bleeding gums, loose or sensitive teeth, painful chewing, and persistent bad breath.
That means the phrase gum disease headache is understandable, even if the headache is often indirect. In real life, people may describe pressure, facial pain, temple pain, or a dull headache when the actual problem starts in the gums, a tooth, or surrounding tissues. Cleveland Clinic notes that tooth-related pain can come with swelling in the gums and headaches, and Mayo Clinic describes dental abscesses and infected oral structures as causes of significant pain and swelling. (Cleveland Clinic)
Table of Contents
What Is Gum Disease?
Gum disease, also called periodontal disease, is an infection or inflammation of the tissues that support your teeth. It usually begins when plaque builds up along and under the gumline. Early gum disease is called gingivitis, and it may cause redness, swelling, and bleeding. If it worsens, it can progress to periodontitis, which can damage the tissues and bone that hold teeth in place.
The symptoms of gum disease often start in the mouth, not the head. According to NIDCR, signs include swollen or bleeding gums, painful chewing, bad breath, sensitive teeth, and gums pulling away from the teeth. So if you have headaches plus these mouth symptoms, it is worth considering that an oral health issue may be contributing. (NIDCR)
Can Gum Disease Cause Headaches?
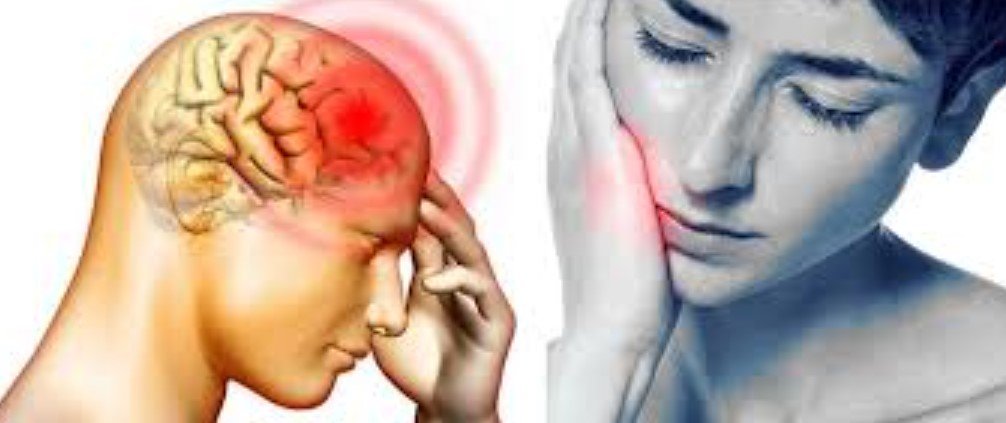
Gum disease can be associated with headaches, but usually not in a simple one-step way. More often, the headache happens because gum inflammation, infection, dental pain, jaw tension, or a localized abscess creates referred pain. A person may feel discomfort in the jaw, cheek, temple, or side of the head instead of only in the gums. Tooth-related pain can include headaches, and oral infections can become painful enough to affect surrounding areas.
So the better answer is this: gum disease may contribute to headache-like pain, especially when there is infection, swelling, painful chewing, or spread of irritation into nearby structures. It is also possible that what feels like “gum disease headache” is actually a tooth infection, a periodontal abscess, an impacted wisdom tooth problem, or jaw-related pain. Mayo Clinic lists jaw pain and swelling among dental problems that can accompany oral infection, and NHS advises prompt dental assessment for ongoing tooth pain. (Mayo Clinic)
How Gum Problems May Lead to Head Pain
Inflammation and pressure in nearby tissues
When gums are inflamed, the surrounding tissues can become sore and swollen. That local irritation may not stay neatly confined to one tiny spot. Pain in the mouth can radiate into the face or head, especially when chewing, clenching, or touching the area makes symptoms worse. NIDCR lists painful chewing as a symptom of gum disease, while Cleveland Clinic notes that dental pain can come with headaches.
Gum infection or periodontal abscess
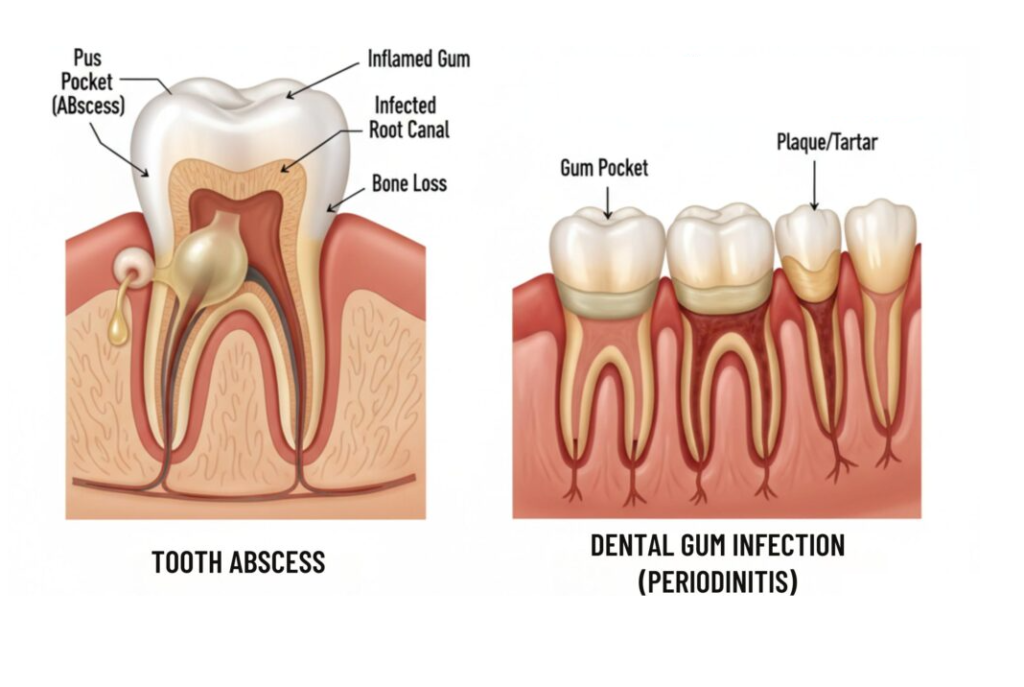
A more serious gum-related problem is an abscess. Dental abscesses are bacterial infections that create a pocket of pus and can cause significant pain, swelling, and spreading discomfort. Mayo Clinic explains that an abscess is caused by bacterial infection and can occur near the tooth or gum, while NHS materials note that infection in a tooth or gum can lead to a painful buildup of pus.
Painful chewing and jaw strain
If gum disease makes chewing painful, people often change how they bite or clench. That can strain the jaw and surrounding muscles, which may contribute to a dull headache or temple pain. NIDCR specifically includes painful chewing among gum disease symptoms, and painful oral conditions are well known to create referred discomfort beyond the original site.
Nearby dental causes mistaken for gum disease
Sometimes a person thinks their gums are causing the headache, but the real cause is a tooth issue, impacted wisdom tooth, or tooth-root infection. Mayo Clinic notes that impacted wisdom teeth can cause red or swollen gums, jaw pain, swelling around the jaw, bad breath, and trouble opening the mouth. Those symptoms can overlap with gum disease and may also lead to head pain or facial pain.
Also Read: Can Gum Disease Cause Bad Breath? Signs, Causes, and Solutions
Signs Your Headache May Be Related to Gum Disease
A headache is more likely to be linked to gum or dental trouble if it happens alongside symptoms inside the mouth. Important clues include swollen or bleeding gums, gum tenderness, bad breath that does not go away, sensitive teeth, painful chewing, gum recession, jaw soreness, or a bad taste in the mouth. These are common signs of gum disease or related dental infection.
You should be even more suspicious of an oral cause if the pain seems focused on one side of the face, worsens when eating, chewing, or biting down, or comes with visible swelling. Toothache guidance from NHS recommends seeing a dentist if tooth pain lasts more than two days, because treating the cause early can stop it from getting worse. (nhs.uk)
What Does a Gum Disease Headache Feel Like?
People describe this type of pain in different ways. It may feel like a dull headache, facial pressure, throbbing near the jaw, pain near the temples, or a one-sided ache that seems to start around the mouth. That variation makes sense because oral pain is often referred rather than perfectly localized. Cleveland Clinic notes that toothache symptoms can include gum swelling and headaches, which supports how dental pain may be felt beyond the tooth or gum itself.
Still, not every headache with sore gums is caused by gum disease. Headaches are common and can happen for many unrelated reasons, while oral symptoms can come from different dental conditions. The best approach is to look at the whole symptom picture rather than assuming every headache with gum discomfort has a periodontal cause.
Gum Disease or Dental Abscess: Why the Difference Matters
This distinction matters because a mild case of gingivitis is very different from a painful infection. Gingivitis is often reversible with improved brushing, flossing, and professional cleaning. But a dental or periodontal abscess is more urgent because it involves active infection and can worsen without treatment. NIDCR says gingivitis caused by plaque buildup can often be reversed with daily brushing and flossing, while Mayo Clinic describes abscesses as bacterial infections that create pockets of pus.
If your “gum disease headache” comes with strong throbbing pain, swelling, fever, a bad taste, or worsening tenderness, the issue may be infection rather than routine gum irritation. In that case, do not rely on home care alone. Dental evaluation is important.
Other Symptoms That Need Quick Attention
Some symptoms should not be brushed off. Seek prompt dental or medical care if you have significant facial swelling, severe pain, pus, fever, trouble opening your mouth, or symptoms that are rapidly getting worse. Swelling in the mouth may indicate a dental abscess, and oral infections can become more serious if ignored.
A severe headache with neurological symptoms such as confusion, weakness, seizures, or vomiting is not typical gum disease and needs urgent medical attention. NHS notes that severe headache with those kinds of symptoms can point to far more serious conditions.
How Dentists Check Whether Gums Are Behind the Headache
A dentist will usually examine your gums, teeth, and bite, check for swelling or infection, ask about bleeding and sensitivity, and look for signs of plaque buildup or deeper periodontal disease. They may also assess whether a tooth infection, wisdom tooth problem, or abscess is the more likely cause of your pain. Mayo Clinic’s periodontal evaluation includes symptom review, mouth examination, and measuring the pocket depth around the teeth when needed.
This matters because the treatment depends on the cause. A cleaning may help if the issue is plaque-related gingivitis, but infection, abscess, or advanced periodontal disease may need more involved treatment.
Treatment for Gum Disease Headache
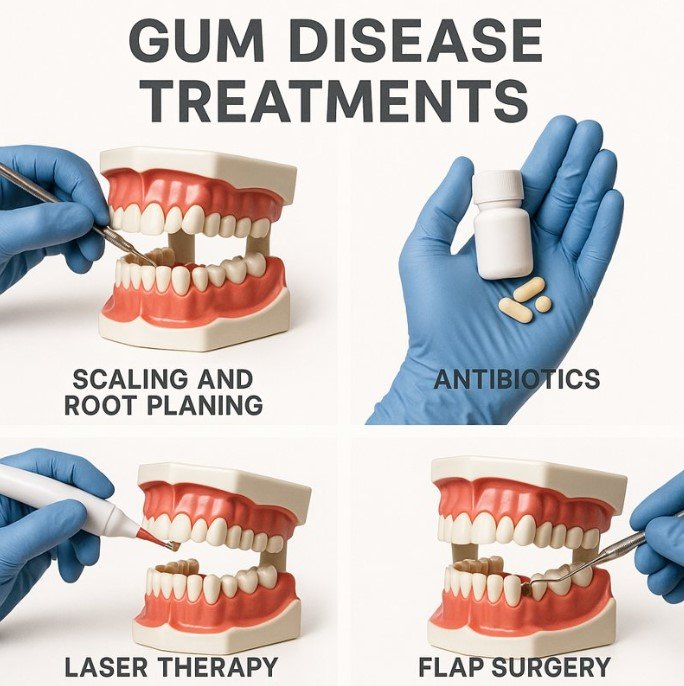
Professional dental cleaning
If plaque and tartar are driving gum inflammation, professional cleaning is often the first step. Removing buildup helps reduce irritation and gives the gums a chance to heal. NIDCR explains that plaque buildup along and under the gumline is a common cause of gum disease.
Better home oral care
Daily brushing and cleaning between teeth are essential. NIDCR states that gingivitis caused by plaque can usually be reversed with regular brushing and flossing. That makes home care one of the most valuable long-term ways to reduce recurring gum inflammation.
Treatment for infection or deep gum pockets
More serious periodontal problems may require deeper treatment to clean beneath the gumline, reduce bacteria, and lower inflammation. Mayo Clinic also notes that subgingival antibiotics like minocycline may be used in periodontal disease because the condition is caused by bacteria beneath the gumline.
Management of abscesses or tooth-root infection
If the pain is caused by an abscess or tooth-root infection, treatment needs to target that infection directly. An abscess will not usually resolve through normal brushing alone. Mayo Clinic and Cleveland Clinic both describe abscesses as bacterial infections that need appropriate dental treatment.
How to Reduce the Risk of Gum Disease and Related Head Pain
The most practical prevention steps are also the simplest: brush thoroughly, clean between your teeth every day, keep up with routine dental visits, and do not ignore bleeding or swollen gums. NIDCR’s oral hygiene guidance emphasizes brushing and cleaning between teeth to remove plaque and reduce the chance of gingivitis.
It also helps to take oral symptoms seriously early. Bad breath that will not go away, painful chewing, sensitive teeth, receding gums, or bleeding gums are not small details. They may be early warnings that something in your mouth needs attention before it becomes painful enough to affect your face or head.
People with diabetes should be especially careful because NIDCR notes that they have a higher chance of periodontal disease, which can lead to pain and healing problems.
When to See a Dentist
See a dentist if you have headaches plus gum bleeding, swelling, chewing pain, gum tenderness, tooth sensitivity, bad breath, or one-sided mouth pain that keeps coming back. Also book an appointment if you think you have toothache or gum pain that has lasted more than a couple of days. NHS advises seeing a dentist when toothache lasts more than two days, and oral infections should not be left to worsen.
Do not wait for the pain to become severe. The earlier the cause is identified, the easier it is to treat gingivitis, periodontal problems, or a developing infection before complications set in.
Final Thoughts
A gum disease headache is possible, but usually indirectly. Gum disease itself is mainly a disease of the gums and supporting structures of the teeth, yet the inflammation, painful chewing, infection, and nearby dental problems that come with it can contribute to facial pain or headaches. The most important takeaway is this: if your headache keeps showing up with swollen, bleeding, tender, or painful gums, do not just treat the head pain and move on. Let a dentist check the mouth, because the source may be periodontal inflammation, a tooth problem, or a dental abscess that needs proper treatment.