Oral Surgery Aftercare Instructions: A Comprehensive Guide
Oral surgery after care instructions protect the blood clot, reduce bleeding, control pain, lower infection risk, and help the extraction site heal in a steady way. These steps matter after Tooth Extraction, wisdom teeth removal, implant work, and other forms of Oral Surgery (OS). Whether your procedure was linked to Orthodontics, a simple extraction, or treatment by Oral Surgeons and Maxillofacial Surgeons, the first few days shape the healing process.
A good oral surgery aftercare plan has clear parts. You protect the wound in the first hour, manage Bleeding and Oozing, control Pain, take oral surgery antibiotics if prescribed, reduce swelling, and keep a safe daily oral hygiene routine. You eat a soft food diet after oral surgery, drink enough water, avoid smoking and alcohol, and watch for warning signs such as pus, worsening pain, or fever. These post-operative guidelines help the gums and teeth recover while lowering the chance of dry socket, infection, and delayed healing.
Many patients search for oral surgery post op instructions, oral surgery home care instructions, or aftercare instructions for oral surgery right after treatment. The reason is simple. The mouth heals fast when the area is protected, kept clean, and not disturbed. The main goal is to preserve the protective blood clot. That clot covers the wound, supports the gums, and acts as the foundation for recovery. Once that clot is lost too early, pain can increase and healing can slow.
Table of Contents
The First Day: Setting the Foundation for Healing
The first 24 hours are the most sensitive part of oral surgery recovery. During this time, your body starts building a protective blood clot over the surgical site. That clot is what shields bone and nerves, limits bleeding, and supports tissue repair. If the clot gets disturbed, the extraction site becomes more vulnerable to pain, infection, and dry socket.
Rest is one of the best things you can do on the first day. Keep your head raised with one or two pillows. Limit talking, avoid bending over, and minimize strenuous activity. Exercise after oral surgery can increase pressure and restart bleeding, so avoid workouts, heavy lifting, and intense movement for at least 48 to 72 hours, or longer if your dentist says so.
Use this first day to stay calm, hydrated, and careful. Drink water in small amounts. Do not use a straw. Suction can pull at the blood clot and disturb the healing site. Small choices during this stage often decide whether recovery feels smooth or painful.
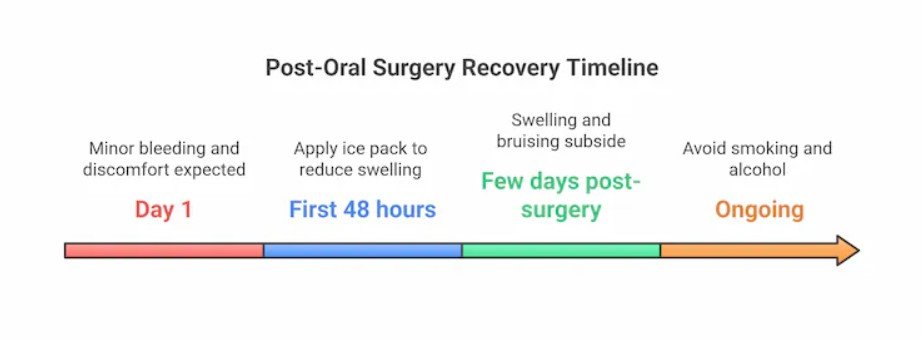
Immediate Post-Operative Instructions (First Hour)
The first hour after surgery is about one thing: steady pressure on the bleeding site. Bite down gently but firmly on the gauze packs placed over the area. Keep the gauze in place for about 30 minutes. If the gauze becomes soaked, replace it with clean gauze and continue applying pressure.
A damp tea bag can help if gauze is not enough. Tea contains tannins that may help the area tighten and reduce bleeding. Place the tea bag over the site and bite down for another 30 to 60 minutes. Make sure the pressure stays directly over the extraction site. If the gauze or tea bag sits in the wrong place, it will not control bleeding well.
Do not eat, drink, rinse, spit, or sleep with gauze in your mouth. The aim during this first hour is simple: allow the blood clot to form without disturbance.
Managing Bleeding and Oozing
Light bleeding and oozing are common after oral surgery. In many cases, what looks like a lot of blood is a small amount mixed with saliva. That is normal. A pink tint in the saliva can continue for several hours, and mild oozing can last up to 24 hours. It may last a bit longer in patients who take blood thinners.
To manage bleeding, place clean gauze over the bleeding site and bite down for 30 to 60 minutes. Sit upright and keep your head elevated. Avoid checking the site too often with your tongue or fingers. Repeated disturbance slows clot formation.
Call your dentist or Oral Surgery Group if bleeding stays heavy, if blood fills the mouth quickly, or if the gauze never comes out lighter after repeated pressure. Heavy bleeding is not the same as mild oozing. The difference matters.
Pain Management
Pain after oral surgery is normal. The level depends on the procedure, your pain threshold, and how closely the area is protected during the first day. The best time to start a pain reliever is before the numbness fully wears off. That often gives more stable relief.
Many dentists recommend ibuprofen, including Advil or Motrin, if your medical history allows it. Acetaminophen, including Tylenol, is another common option. Some patients receive a narcotic for stronger pain after more involved surgery. Take every medicine exactly as directed. Use food when allowed, since that can reduce stomach upset and nausea. If a narcotic makes you sleepy, do not drive or operate machinery.
Do not take aspirin unless your dentist or surgeon specifically tells you to use it. Aspirin can increase bleeding in some cases. Pain should improve day by day. Call your dentist if the pain becomes stronger instead of weaker after the first few days.
Antibiotics and Infection Prevention
Oral surgery antibiotics are not given in every case, though they are sometimes prescribed to treat or prevent infection. If your dentist gives antibiotics, finish the full course exactly as directed. Stopping early can allow bacteria to return and may reduce the benefit of treatment.
Watch for allergic or adverse reactions. These can include rash, itching, nausea, swelling of the lips, or trouble breathing. Trouble breathing needs urgent medical care. Mild stomach upset can happen with antibiotics, so taking the medicine with food may help if your dentist says that is appropriate.
Infection prevention is not only about medicine. It is also about keeping the blood clot stable, avoiding smoking, keeping the mouth clean in a gentle way, and following a soft food diet after oral surgery. Good after surgery care reduces the chance that bacteria will enter the wound.
Swelling Reduction
Mild swelling and pain are a normal part of oral surgery aftercare. Swelling usually rises during the first 24 to 48 hours and then starts to settle. You can reduce it with a cold compress on the cheek. A common routine is 30 minutes on and 30 minutes off during the first 24 to 48 hours.
Keep your head elevated when resting or sleeping. That simple step helps fluid drain and may reduce facial swelling. After the first 48 hours, warm compresses can feel better and may help the swelling go down more quickly.
Call your dentist if swelling keeps increasing after 2 to 3 days, becomes very hard, or comes with fever, pus, or a bad taste. Those signs may suggest infection rather than routine swelling.
Oral Hygiene: Keeping Your Mouth Fresh and Clean

A clean mouth heals better, though the cleaning must stay gentle. On the day of surgery, avoid disturbing the treated area. You can still care for the rest of your mouth. That means a careful daily oral hygiene routine, gentle brushing away from the surgical site, and no harsh mouthwash.
The goal is to keep bacteria under control without pulling on the blood clot. That is why alcohol-based rinses are a poor choice during early healing. Alcohol can dry the tissues and irritate the wound. Warm salt water is usually a better option once your dentist says you can start rinsing.
A soft-bristled toothbrush and fluoride toothpaste are useful during this stage. General dental care does not stop after surgery. It just becomes more careful for a short time.
Rinsing
Avoid rinsing for the first 24 hours unless your surgeon gave different instructions. Early rinsing can disturb the clot and restart bleeding. After the first day, start gentle warm salt water rinses. Mix 1 teaspoon of salt in 8 ounces of warm water, which is about 240 mL. Rinse softly 3 to 4 times a day, especially after meals.
Gentle saltwater rinses help remove food and reduce bacterial buildup without the harsh effect of some commercial mouthwashes. Use warm salt water, not hot water. Hot liquid can irritate the wound and increase bleeding.
This step sounds small, though it is one of the most useful parts of oral surgery aftercare. It keeps the area fresh while protecting the healing site.
Spitting
Do not spit forcefully after oral surgery. Forceful spitting creates pressure in the mouth, and that pressure can dislodge the blood clot. The same rule applies to sucking through a straw, forceful rinsing, and repeated clearing of the mouth.
If saliva builds up, let it fall out gently or swallow carefully if your dentist has not told you otherwise. Saliva mixed with a little blood can look alarming, though that does not always mean active bleeding. The safest approach is simple: avoid force.
Brushing
Begin brushing again as soon as you can do so comfortably, though keep the brush away from the surgical site on day one. Clean the rest of the teeth gently with a soft-bristled toothbrush. Use fluoride toothpaste to support general dental care and protect the other teeth while you recover.
On the second day and after, you can carefully clean closer to the area if it does not cause pain and if your dentist approves. Do not scrub the gums. Do not poke stitches. Think gentle contact, not aggressive cleaning.
Colgate and similar dental care brands often suggest soft brushing after dental treatment, and that advice fits well here. The brush should clean the mouth, not disturb the wound.
Also Read: Order of Oral Care: Best Routine for a Healthier Smile
Irrigation Syringe Use
Some patients receive an irrigation syringe after surgery, especially after wisdom tooth removal. If your surgeon gives you one, do not use it too early. Many offices advise starting about 1 week after surgery, once the socket is more stable.
Fill the syringe with warm water and flush the area gently after meals. The purpose is to remove trapped food from the hole as it heals from the bottom upward. It is normal to feel a small opening for a while. That space closes gradually over several weeks, and deeper bone healing takes longer.
Do not use the syringe with force. The goal is to rinse debris out, not to blast the tissue. If you are unsure about timing, call your dentist before using it.
Diet and Nutrition: Eating Soft Foods That Help You Heal
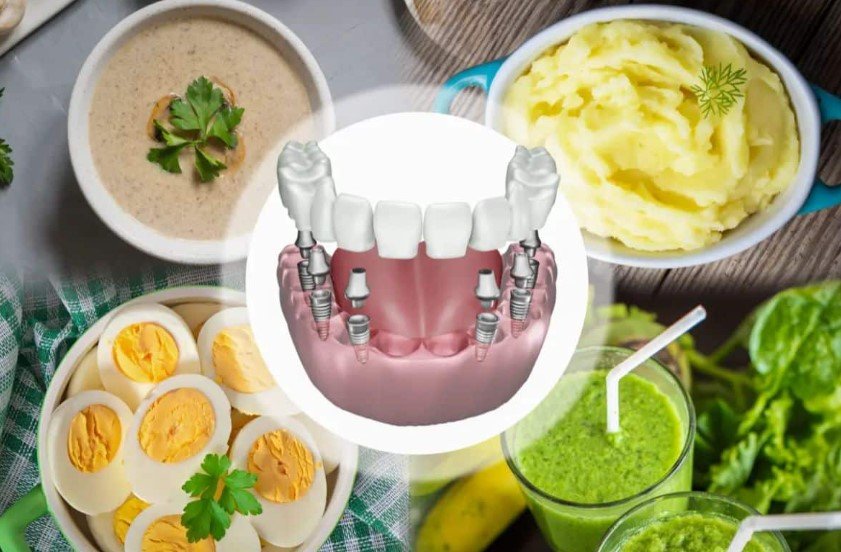
A soft food diet after oral surgery keeps pressure off the gums and makes eating less painful. Good first choices include yogurt, mashed potatoes, smoothies eaten with a spoon, applesauce, pudding, lukewarm soups, and soft scrambled eggs. These foods are easy to manage and can help you maintain energy while the mouth is sore.
Stay away from crunchy, hard, spicy, hot, or seedy foods. Avoid nuts, seeds, popcorn, chips, rice, and corn near the early healing stage. These foods can irritate the wound or get stuck in the socket. Avoid drinking through a straw for at least 1 week, since suction can disturb the blood clot.
Hydration promotes healing. Water should be your main drink. Cool or room-temperature drinks often feel best during the first day. Eat regular meals if you can. A restricted diet initially is normal, though skipping food completely can make pain, weakness, and nausea worse.
Nausea Management
Nausea can happen after oral surgery from swallowed blood, pain medicine, antibiotics, or an empty stomach. Small sips of water may help. Some offices suggest a carbonated drink such as ginger ale or cola in small amounts every 30 minutes until nausea settles. Saltine crackers may help too when you are ready for food.
Take medicine with food if your instructions allow it. That often reduces stomach upset. Keep meals bland and simple during this stage. If nausea continues, if vomiting starts, or if you cannot keep fluids down, call your dentist.
Medication adherence is essential, though safe recovery matters more. If medicine is making you sick, ask the office for guidance rather than stopping or guessing.
Understanding and Preventing Dry Socket
Dry socket is one of the main complications patients worry about. It happens when the protective blood clot is lost too early from the extraction site. Without that clot, the bone and nerves are exposed. The result is pain that can feel strong, deep, and constant.
Dry socket pain often starts on day 3 or day 4 after surgery, not right away. The pain may spread to the ear, jaw, or nearby teeth. The socket may look empty or have a bad smell. The gums around it can still look fairly normal, which is why patients sometimes miss the cause.
You can help prevent dry socket by avoiding smoking, straws, forceful rinsing, forceful spitting, and hard activity in the early days. Keep the site clean with gentle warm salt water once allowed. If pain increases sharply after a few days, contact your dentist. The Mayo Clinic describes dry socket as a painful complication after extraction, and prompt treatment can bring relief.
Smoking and Alcohol: Habits That Support Healthy Healing
Do not smoke after oral surgery. Smoking slows blood flow, irritates the wound, raises infection risk, and increases the chance of dry socket. Avoid smoking entirely for at least 1 week, and longer is better if you can manage it. Chewing tobacco has similar risks and should be avoided too.
Avoid alcohol while you are taking antibiotics or pain medicine. Alcohol can interfere with healing, increase dryness, and react badly with certain medicines. It can make dizziness and nausea worse as well.
This part of oral surgery care instructions sounds strict, though it is one of the clearest ways to support recovery. Healthy healing needs a clean, stable environment.
Sharp Bony Edges
After Tooth Extraction, you may feel something hard near the gums and think a piece of tooth was left behind. In many cases, that hard area is a sharp bony edge from the bone that once supported the tooth. Small bone irregularities can be felt by the tongue during healing.
Do not pick at the area. Leave it alone and let your dentist assess it if it becomes painful or does not settle. Many of these spots smooth out as the gums heal. Some need a simple adjustment by the dentist if they stay exposed.
Patients often worry when they feel something rough. That concern is common. The best step is observation, not self-treatment.
Easing Discomfort While You Recover
Recovery feels easier when you support the whole body, not just the mouth. Rest well. Drink enough water. Stay with a soft food diet after oral surgery. Use your cold compress or warm compress at the right stage. Take medicine on time instead of waiting for pain to become severe.
Avoid strenuous activity for a few days. Minimize strenuous activity until bleeding has stopped, swelling is settling, and you feel steady. Healing tissue does better when blood pressure and movement stay moderate. Keep your head elevated and give yourself time.
Patients often ask how long gums take to heal. Surface healing usually starts to look better in 1 to 2 weeks. Deeper healing of the socket and bone can take several weeks to several months, depending on the procedure and your general health. Patience matters. Healing does not happen all at once.
When to Seek Help
Call your dentist or surgeon if you notice any of these problems:
- heavy bleeding that does not slow with pressure
- swelling that keeps getting worse after 2 to 3 days
- fever
- pus or a foul-tasting discharge
- trouble breathing or swallowing
- severe pain that starts or becomes much worse on day 3 or day 4
- rash, itching, or swelling after antibiotics
- vomiting that prevents you from keeping fluids down
These are the signs that go beyond normal oral surgery recovery. Most patients heal without major trouble, though early contact is always better than delayed care. This is true in General practice, specialist settings, and clinics across Australia and other regions.
Taking Care of Your Smile After Recovery

Once the wound has closed and your dentist says healing is on track, return fully to your regular general dental care routine. Brush twice a day with fluoride toothpaste, floss as directed, and keep follow-up visits. Good habits protect the teeth, gums, and any future dental work.
Recovery is a good time to reset oral health habits. Replace an old toothbrush. Keep dental checkups on schedule. Watch sugar intake. Stay hydrated. Small habits support long-term comfort.
If your procedure was part of a wider treatment plan, such as Orthodontics, implants, or staged oral surgery, follow every follow-up appointment. Long-term results depend on what happens after the procedure as much as during it.
Referral Sites:
https://medlineplus.gov/ency/article/007630.htm
https://www.geh.nhs.uk/patients-and-visitors/patients/patient-leaflets/post-operative-instructions-after-extraction
https://www.mayoclinic.org/diseases-conditions/dry-socket/diagnosis-treatment/drc-20354382
https://www.nidcr.nih.gov/health-info/opioids
Final Thought
Oral surgery after care instructions work best when you protect the blood clot, control pain, keep the mouth clean in a gentle way, follow a soft food diet, and avoid habits that disturb healing. These steps reduce bleeding, lower infection risk, and help the extraction site recover with fewer problems.
The first few days need the most care. Use gauze packs when needed. Choose warm salt water after the first day. Use a soft-bristled toothbrush and fluoride toothpaste carefully. Avoid smoking, alcohol, and straws. Call your dentist if pain worsens, pus appears, or swelling keeps rising.
That is the core of good oral surgery aftercare. Keep the site protected, keep the routine gentle, and give the gums time to heal.